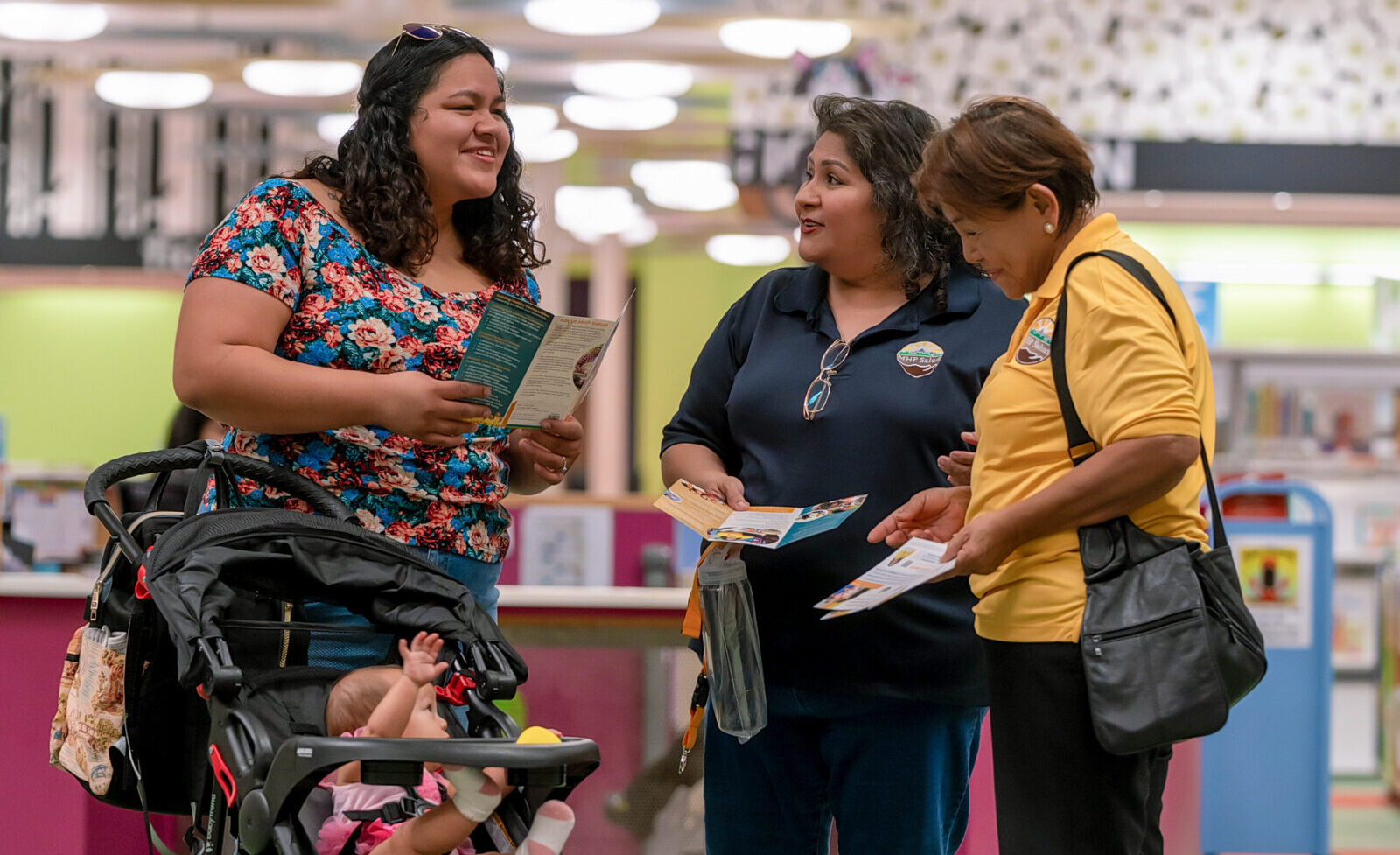A Healing Works Grantee Spotlight
Thanks to MHP Salud, community health workers are connecting Florida and South Texas residents with whole person care. CEO Magaly “Maggie” Dante, PhD, shares the story of one young man, who reached out for food stamp help. In talking with him, a community health worker (CHW) learned that he didn’t have health insurance. He thought he didn’t need it, because he was young and healthy.
The CHW kept the conversation open. Months later, she encountered him on his way to take his dog to the veterinarian. “Your own health is just as important,” she said. “And if you don’t take care of yourself, who will take care of your dog?”
That everyday encounter resonated, and the young man accepted help to find health insurance and get a checkup. Within days, he learned his blood sugar was off the charts—he had diabetes, which he would never have known about without his CHW building trust.
A solution to improve care
If you’re a primary care clinician serving low-income communities, you know the challenge. Your patients face barriers beyond the exam room—transportation difficulties, language barriers, insurance confusion, food insecurity, even social isolation. They may be like the young man Dante describes, thinking they don’t need health care when, in fact, they need comprehensive support. Fifteen-minute appointments don’t allow enough time to build a relationship of trust and mutual respect.
As the story shows, CHWs can offer a solution. They are public health workers who often come from the communities they serve, so they share an ethnic background, culture or language and a bond of trust. They understand the social factors that drive health for those around them.
Getting CHWs involved in care is an important way to practice whole person health. Workers can provide person-centered, relationship-based care that addresses the social, spiritual, emotional, and behavioral aspects of patients’ health.
Our team at the Healing Works Foundation partners with several organizations around the United States aligned with our mission of making whole person, integrative care regular and routine. MHP Salud is one of our recent grantees and has an established track record with 40 years of impact. This organization leads the way in training and utilizing CHWs for whole person care both in primary care and cancer care.
Meet MHP Salud
Currently, MHP Salud is working in a total of 10 counties, serving communities in South Texas and Central Florida and training others in almost every state. It has a dual mission: providing direct community services while building the CHW workforce nationally. They serve as both practitioner and teacher, constantly refining best practices grounded in research and experience.
Dante recalls being the only Spanish-speaking clinician in rural Florida and realizing that a whole health approach was essential. “I had a client who was 21, HIV-positive, pregnant, and on public assistance. She couldn’t pay rent and had no childcare help. Getting her regular checkups wouldn’t address those problems.”
This experience helped shape MHP Salud’s approach of addressing complete life contexts, not just medical needs.
A hidden healthcare crisis
In Texas’ Rio Grande Valley, MHP Salud serves communities where 41% are uninsured, 63% have household incomes below $25,000, and health statistics are stark: 55% obesity, 39% hypertension, 32.5% diabetes. Texas has the highest rate of uninsured children in the United States—12% compared to 5% nationally.1
Insurance alone doesn’t solve the problem. In the areas where MHP Salud works, other issues keep patients from getting needed care. For example, communities in Florida face a shortage of clinicians. Rural communities in Texas struggle with transportation and, again, a clinician shortage.
But perhaps most overlooked is trust. People from more economically or socially vulnerable populations may avoid care after having negative experiences. Language and cultural differences can add to patients’ distrust, resulting in delayed care, a reliance on the emergency department, and chronic disease progression.
How CHWs help
From a clinical support standpoint, CHWs provide outreach, home visits, health education, and care management. From a whole person standpoint, they also function as cultural mediators between specific communities and the world of health care.
When community members begin to trust the clinicians and resources available to them, they can seek out care, often with a CHW’s help and encouragement. CHWs help patients navigate complex systems, whether they are using telemedicine for the first time, finding an interpreter, or searching for low-cost rides to a specialist in an urban area.
While they can’t replace clinicians, CHWs enhance quality. They coordinate, help relieve clinicians’ overwork and burnout potential, and foster patients’ and families’ trust.
Measurable impact
MHP Salud’s 2025 results demonstrate whole person health principles in action. Here are some highlights:2
- The Navigator program (which helps individuals sign up for insurance) served 2,234 consumers, securing 2,050 health plans with 77.8% approval rate.
- Through Connecting Kids to Coverage, 982 children and parents enrolled in Medicaid and CHIP.
- The Parents as Teachers program engaged 234 families with 69% retention for at least a year.
- Familias Saludables reached 995 families to improve nutrition and health.
- Amaté/SHADE HIV prevention served 165 youth, achieving 97% increased knowledge and 90% improved attitudes.
In 2025, they reached 1,609 health professionals through national training events, with hundreds of federally qualified health centers participating. Nearly half of all CHWs certified in Florida were trained by MHP Salud.
At MHP Salud, over 90% of clients come through word of mouth, demonstrating trust and satisfaction.
This illustrates the effectiveness of CHWs: lived experiences enrich their work, enabling deeper community connections that lead to better health.
The evidence
Research consistently demonstrates that CHWs help whole person health. A 2023 systematic review found CHWs enhance quality of care, facilitate coordination, alleviate clinician burdens, and foster trust.3 Evidence shows CHWs improve diabetes outcomes,4 proved instrumental during the COVID-19 pandemic,5 and demonstrated effectiveness as vaccinators.6
Financially, evidence-based CHW programs generate positive returns by helping reduce hospitalizations and use of emergency departments.7,8 CHWs don’t just provide information—they alter how patients engage with care. They can help patients move from avoiding your office to proactively seeking care.9
Benefits for health care organizations
CHWs address another challenge in health care: clinician burden and staff retention. Turnover in public health has reached crisis levels—50% on average, rising to 70% among professionals with under five years’ experience. Research shows turnover negatively impacts patient outcomes.10
MHP Salud’s experience proves the point. Five years ago, their annual turnover was 47%. By focusing on workplace culture, trauma-informed approaches, reflective supervision, individualized development, and meaningful meetings, they reduced turnover to 11%—saving nearly $1 million annually while dramatically improving work quality.
Getting started
If you’re interested in implementing CHWs, resources exist. Most states have CHW associations and certification processes. The National Association of Community Health Centers provides training and assistance. MHP Salud offers comprehensive workforce development training, customized consulting, and apprenticeship programs.
Success requires a commitment that goes beyond just hiring more staff. As MHP Salud’s own story shows, organizations need a strong culture of support, a focus on retention, and a commitment to developing staff in meaningful ways. CHWs are trusted professionals whose experiences and connections qualify them to bridge gaps traditional health care cannot.
A way to build bridges
As health care trends toward population health and value-based care, CHWs provide a model of lowering barriers, reducing disparities, and transforming the patient experience.
MHP Salud’s work illustrates how CHWs can bridge the gap between health systems and communities. They provide time, build relationships, validate community knowledge, and offer culturally competent support for body, mind, and spirit.
If you’ve been frustrated patients can’t or don’t access care despite your efforts, if your community needs more than traditional models provide, or if you’re committed to advancing whole person health—CHWs and partnerships with organizations like MHP Salud are well worth exploring.
Resources
MHP Salud: https://mhpsalud.org, email: info@mhpsalud.org, phone: (956) 968-3600
National Association of Community Health Centers: https://www.nachc.org
References
- MHP Salud. Nonprofit aims to spur health coverage through Mid-Valley location. Updated October 22, 2025. Accessed February 3, 2026. https://mhpsalud.org/2024/09/10/nonprofit-aims-to-spur-health-coverage-through-mid-valley-location/.
- MHP Salud. Our Impact. 2025 Mid-Year Impact Report. Accessed February 3, 2026. https://mhpsalud.org/impact/.
- Knowles M, Crowley AP, Vasan A, Kangovi S. Community Health Worker Integration with and Effectiveness in Health Care and Public Health in the United States. Annu Rev Public Health. 2023;44(1):363-381. doi:10.1146/annurev-publhealth-071521-031648
- Kane EP, Collinsworth AW, Schmidt KL, et al. Improving Diabetes Care and Outcomes with Community Health Workers. Fam Pract. 2016;33(5):523-528. doi:10.1093/fampra/cmw055
- Oliver J, Ferdinand A, Kaufman J, Allard N, Danchin M, Gibney KB. Community Health Workers’ Dissemination of COVID-19 Information and Services in the Early Pandemic Response: A Systematic Review. BMC Health Serv Res. 2024;24(1):711. doi:10.1186/s12913-024-11165-y
- Gibson E, Zameer M, Alban R, Kouwanou LM. Community Health Workers as Vaccinators: A Rapid Review of the Global Landscape, 2000-2021. Glob Health Sci Pract. 2023;11(1):e2200307. doi:10.9745/GHSP-D-22-00307
- Kangovi S, Mitra N, Grande D, Long JA, Asch DA. Evidence-Based Community Health Worker Program Addresses Unmet Social Needs and Generates Positive Return On Investment. Health Affairs. 2020;39(2):207-213. doi:10.1377/hlthaff.2019.00981
- Cardarelli R, Bausch G, Murdock J, Chyatte MR. Return-on-Investment (ROI) Analyses of an Inpatient Lay Health Worker Model on 30-Day Readmission Rates in a Rural Community Hospital. J Rural Health. 2017;34(4):411-422. doi:10.1111/jrh.12250
- Kangovi S, Mitra N, Norton L, et al. Effect of Community Health Worker Support on Clinical Outcomes of Low-Income Patients Across Primary Care Facilities: A Randomized Clinical Trial. JAMA Intern Med. 2018;178(12):1635-1643. doi:10.1001/jamainternmed.2018.4630
- Moscelli G, Mello M, Sayli M, Boyle A. Nurse and Doctor Turnover and Patient Outcomes in NHS Acute Trusts in England: Retrospective Longitudinal Study. BMJ. 2024;387:e079987. doi:10.1136/bmj-2024-079987
Photo from MHP Salud